
When Did This Tumour Start? The need for a Gompertzian Understanding of Tumour Growth Kinetics
Tumour growth is conventionally understood to follow exponential kinetics in many medico-legal courts and summaries. According to this model, the time required for one cell to divide into two is equivalent to that required for two to form four, four to form eight, and so forth. As such, people from claimants to plaintiffs, physicians to patients, and scientists to laymen alike mistakenly assume that, upon determining the doubling time of a hepatic tumour, to give a typical example, the tumour would have likely been present “years ago” in the liver, and the cancer was thus “incurable” years ago. Alas, some say, there was no point in screening, testing, and diagnosing the primary tumour earlier, as it was fatal all along, owing to its metastatic spread. In other words, the patient’s tumour was metastatic well in advance of diagnosis and, hence, there would not have been any prospect of cure with earlier detection.
However, this is incorrect and not the case. After all, we employ two-week waits and screening programs for good reason, and acknowledge dissimilar biologies in different, often heterogeneous tumours. And, if we are going to be purists about it, no two cells are identical, so certainly, no two cancers are. All oncologists have seen ‘good pancreatic cancers and terrible breast cancers.
In reality, the exponential growth model is obsolete. Tumour growth proceeds in a sigmoidal fashion (S-shaped curve) as described by the Gompertz function, developed by British actuary Benjamin Gompertz in 1825[1]. Pursuant to Gompertzian kinetics, tumour growth decelerates as the tumour increases in size, ultimately converging to a carrying capacity. Hence, a fundamental difference between these two models is that an exponential function, being unbounded, suggests that there is no theoretical limit to the size of tumours, which is not pragmatic in vivo, or one should say in reality.
Though the Gompertz function was devised to portray human mortality, it has since been utilised across several disciplines concerning biological growth, including population biology and tumour kinetics, and should evidently be used in cases of medical law. It differs from a simple logistic function in that the curve converges to the carrying capacity more gradually than the lower asymptote.
In 1964, A.K. Laird demonstrated that the growth of several tumours across model organisms could also be aptly described by Gompertzian kinetics[2]. In her study, Laird notes how exponential tumour growth is short-lived and that, when monitored over a comprehensive timescale, tumour growth, in fact, slows down as tumour size increases. This is consistent with the original Gompertzian curve, which is characterised by quasi-exponential growth initially, followed by a decline in growth rate as a carrying capacity is approached. Thus, while the exponential model may delineate initial stages of tumour growth well, it does not paint the full picture or barely the picture at all. This is illustrated in Figure 1:
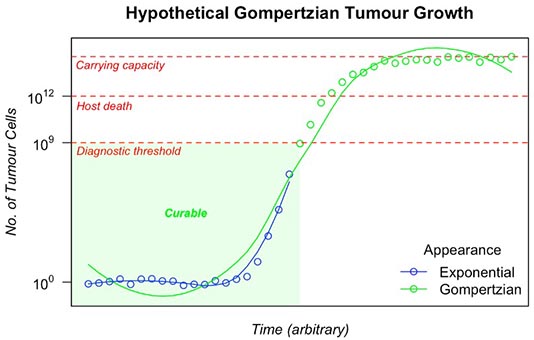
Figure 1. Initial tumour growth at the inflection point appears exponential, despite an overall Gompertzian trend.
Therefore, instances where exponential tumour growth is observed may arise because the patient succumbs to cancer before this carrying capacity is approached, or rather we think the tumour is growing exponentially when in fact it is not. In clinical reality, below the diagnostic threshold and up to a specific time point, the tumour is curable with no obvious metastatic disease despite there often being micro-metastatic cells elsewhere (see Figure 1). After all, to give another example, we often give chemotherapy, as in the case of breast, lung, or colon cancer, when there is no obvious disease after surgery that’s visible to kill those few remaining cells. Moreover, this approach of surgery in conjunction with chemotherapy in stage II or III tumours is usually curative. At the same time, some cancers present with advanced metastatic disease, and at presentation are genuinely incurable.
Importantly, discriminating between these growth models bears significant clinical and medico-legal implications, including accurately predicting the progression of tumours in retrospect[3] and, going forwards, the effect of chemotherapy on the rate of cytoreduction. The log-kill hypothesis, which assumes exponential growth, states that the rate of cytoreduction in response to chemotherapy is constant, irrespective of tumour size[4]. This model also suggests that, given enough doses of chemotherapy, a complete cure can hypothetically be achieved, which is not representative of those with advanced cancer.
Indeed, Larry Norton and Richard Simon conceived a model predicated on Gompertzian kinetics – the Norton-Simon hypothesis – which states that chemotherapy results in a rate of cytoreduction that is directly proportional to the rate of growth of an unperturbed tumour of that size; that is, smaller tumours exhibit greater cytoreduction in response to chemotherapy due to their exponential growth rate[5].
This comprehension of tumour growth dynamics acknowledges that, regardless of when chemotherapy is administered, the outcome with regard to tumour size is effectively identical due to the exponential regrowth of smaller tumours. Subsequently, Norton and Simon theorised that the efficacy of chemotherapy might be enhanced by delivering dose-dense treatments (i.e., at a greater rate), thereby diminishing regrowth between doses5. Citron et al. examined the notion of adjuvant dose-dense chemotherapy in a large clinical trial, whereby patients with node-positive breast cancer were randomly chosen to follow either a dose-dense two-week inter-treatment interval or the customary three-week interval[6]. In accordance with the Norton-Simon hypothesis, the dose-dense cohort exhibited a statistically significant improvement in disease-free survival (P = .010) and overall survival (P = .013) following a median three-year follow-up.
This is a real-life example of research stemming from a Gompertzian understanding of tumour growth being associated with improved clinical outcomes among cancer patients.